Healing Abutments
- Graham Carmichael

- Feb 12
- 2 min read
There are many variables which influence the successful outcome for a patient receiving a dental implant, and not all of these are controllable by the surgeon. Medical co-morbidities, bone quantity or quality, certain medications and the host response may be out of our control, however the surgeon has absolute control of the surgical technique and what components are used.
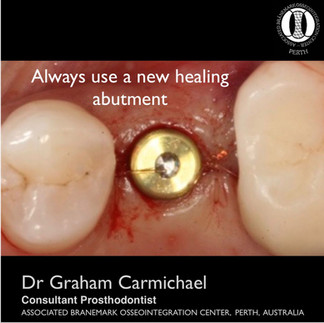
The implant should be supplied by the implant manufacturer pre-sterilised and in appropriate packaging to avoid bacterial or other contamination which could affect the osseointegration of the implant. The trans-mucosal healing abutment placed onto the implant at the time of surgery also needs two be sterile and contaminant free, as this component is vital in protecting the healing implant. It is critical that a new healing abutment is used every time.
A new titanium healing abutment provides the ultimate surface for connective tissue and junctional epithelial integration providing protection from bacterial penetration and oral epithelial down growth towards the head of the implant. This tissue is ruptured when the healing abutment is removed for impression taking or restoration placement, and careful handling of the abutment is necessary to promote a favourable cellular response afterwards.
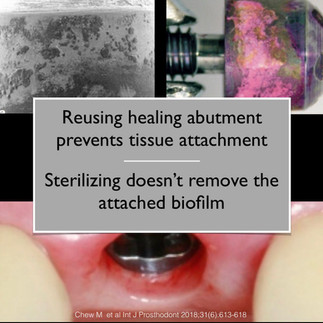
Once a healing abutment has been placed onto an implant, cellular adhesions that form are not removed by dental autoclaving, and this biofilm prevents favourable healing if a healing abutment is reused on the same or different patient. Oral epithelium can migrate to the head of the implant and healing abutment interface, affecting bone attachment height and increase the risk of peri-implant disease.
Every implant should have a new healing abutment placed to promote the optimal environment for healing, and outcome for the patient.










Using a new healing abutment each time makes sense to ensure proper healing; reusing them could compromise patient outcomes significantly. https://iguessbro.com